MKM architecture + design named to BD+C’s 2025 Top Hospital Facility Architecture Firms for its patient-centered, purpose-driven healthcare design.

Workplace violence (WPV) is a pervasive and underrecognized hazard in healthcare. It includes acts or threats of physical violence, harassment, intimidation, or disruptive behavior that occur within a healthcare facility, often affecting not only healthcare workers, but patients, families, and visitors. The consequences are far-reaching, leading to trauma, burnout, and job dissatisfaction among staff prompting many to leave the profession entirely. In 2023, 80 percent of nurses reported experiencing workplace violence, and nearly one in five had already changed jobs or exited healthcare as a result. The downstream effects threaten the stability of the healthcare system, undermining staff retention, eroding public trust, and ultimately compromising patient care.
The built environment plays a critical role in either escalating or mitigating the risk of workplace violence. Poorly designed spaces characterized by confusion, noise, lack of privacy, and limited staff visibility can exacerbate stress and increase the potential for violence. Conversely, more intentional design can serve as a powerful tool for emotional regulation, de-escalation, and safety. Design decisions in healthcare facility environments can either contribute to opportunities for workplace violence or help prevent it by prioritizing staff safety and stress management.
Empathy as a Standard
Architecture is not neutral—it shapes daily experiences and communicates care and respect. Empathy must guide the design process; beginning with understanding the lived realities of healthcare workers, who often operate in high-stress, high-risk settings such as emergency departments and behavioral health units. By acknowledging their experiences and collaborating with staff and stakeholders, designers can create environments that genuinely support safety and well-being.
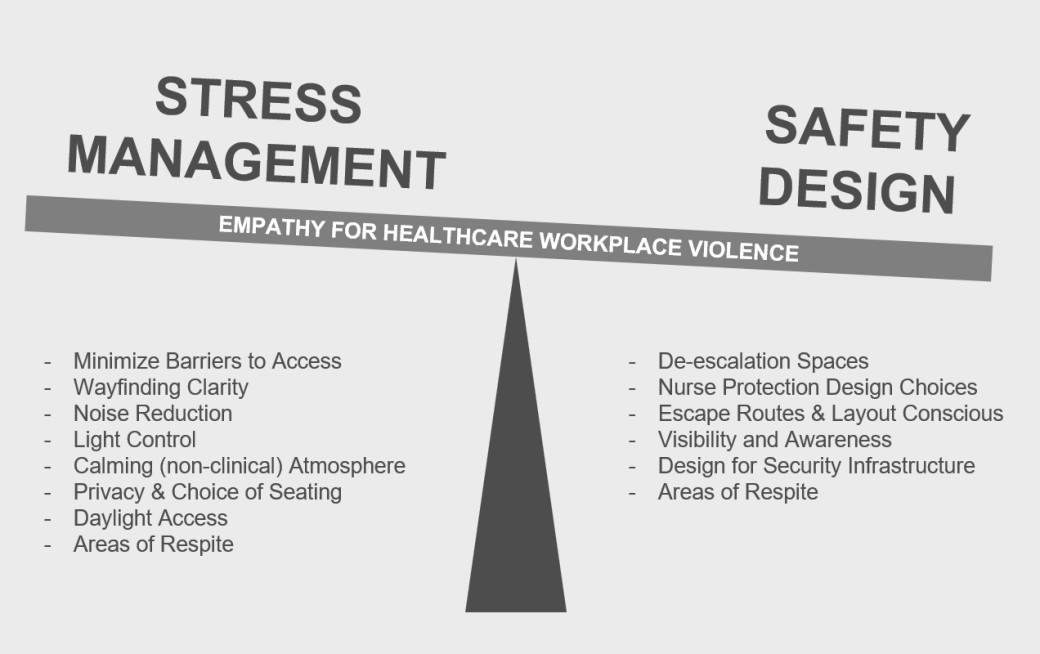
Effective healthcare design balances stress management with intentional safety strategies. Stress-reducing features such as clear wayfinding, noise reduction, access to daylight, privacy, calming aesthetics, and areas of respite help lower anxiety for patients and visitors. Simultaneously, safety-driven choices—like de-escalation spaces, clear escape routes, improved visibility, and integrated security infrastructure—protect staff without making spaces feel punitive or institutional.
Framework for application
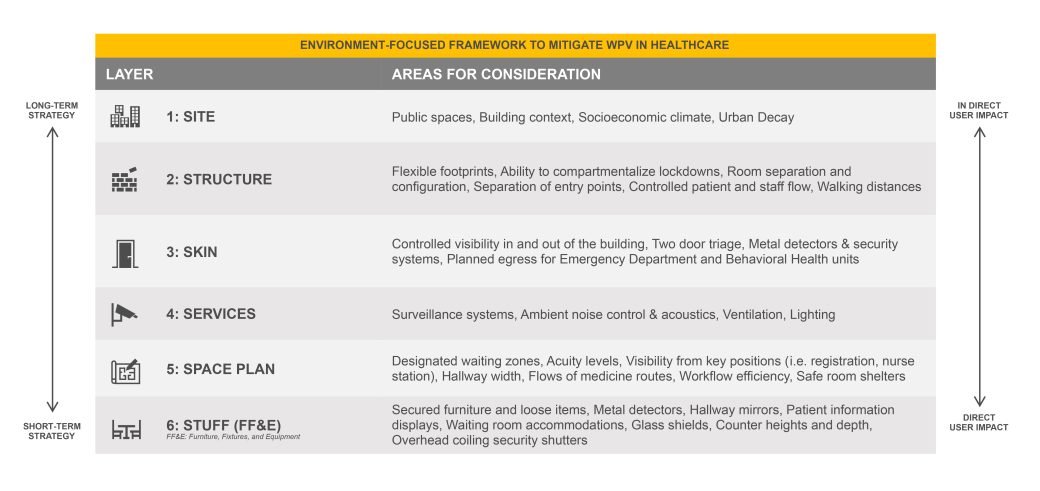
Stewart Brand’s “Shearing Layers” model offers a comprehensive framework for embedding safety and empathy across all aspects of a healthcare facility. Safety can be considered at every layer, from site planning and structural decisions to space planning and furniture selection. While some elements are difficult to change, others—like layouts and furnishings—offer opportunities for adaptability as needs evolve.
Designers Responsibility
Ultimately, healthcare worker safety must become a central concern for architectural designers. The built environment directly influences exposure to violence, stress, and error. By designing spaces that protect staff and reduce stress for everyone, architects play a vital role in strengthening the healthcare workforce, improving care, and building more resilient systems. Designing with empathy is not just a best practice—it is an ethical imperative.
For further reading:
Author, HCD Guest. “Designing for Staff Safety in Healthcare Facilities.” HCD Magazine, December 4, 2023. https://healthcaredesignmagazine.com/trends/applying-behavioral-health-design-strategies-to-other-healthcare-service-lines/62390/.
Jacob, Darren, Belinda Jacob, Elisabeth Jacob, and Alycia Jacob. “Effectiveness of Environmental Design Interventions to Reduce Aggression and Violence in Emergency Departments: A Scoping Review.” HERD: Health Environments Research & Design Journal 18, no. 4 (July 7, 2025): 26–42. https://doi.org/10.1177/19375867251351027.
Mahmoudi, Ali, and Gabriel Castelblanco. “Concept Development of Framework for Workplace Violence Prevention through Building Components Modifications in Hospitals.” Purdue e-Pubs, 2025. https://docs.lib.purdue.edu/cib-conferences/vol1/iss1/33/.